Picture this: a 74-year-old retired teacher named Margaret visits her doctor after years of managing her blood pressure with the same medication prescribed back when smartphones were barely a thing. Her numbers look “okay” — 148/88 mmHg — but she’s been feeling dizzy in the mornings, and her cardiologist just flagged something new. Sound familiar? This scenario plays out millions of times a year, and here’s the thing — what we knew about hypertension management in older adults even five years ago has shifted significantly by 2026.
Let’s think through this together, because the latest research isn’t just academic — it directly affects daily quality of life, fall risk, cognitive health, and longevity for seniors and their families.
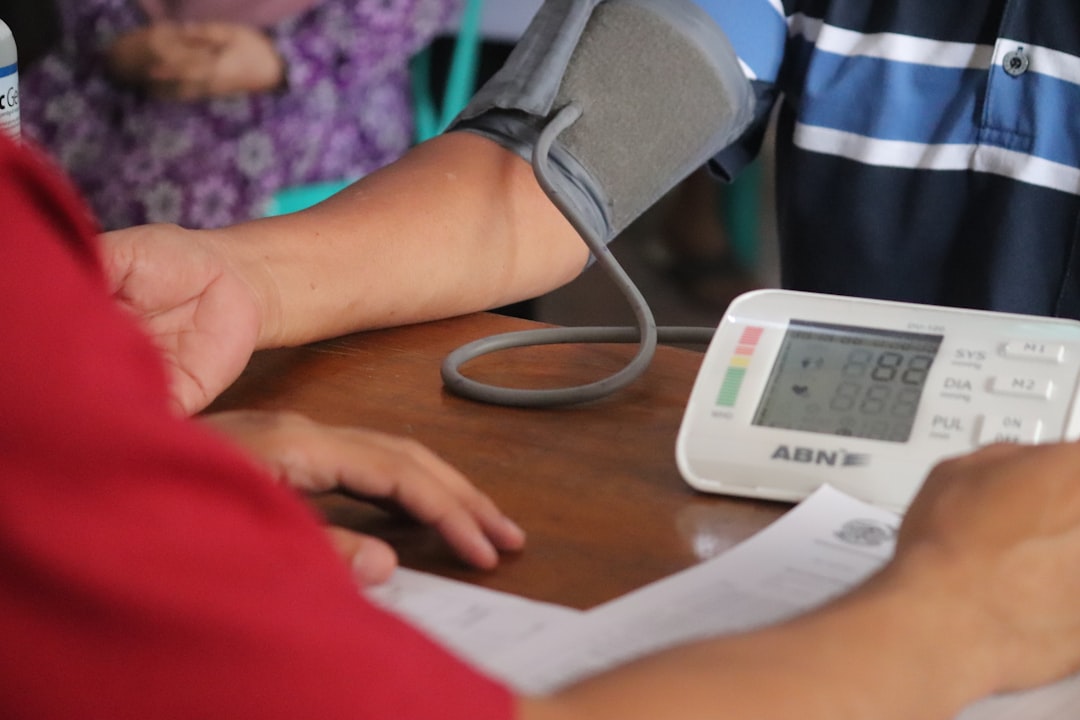
Why Hypertension in Seniors Is a Unique Clinical Challenge
Hypertension — chronically elevated blood pressure — is not a one-size-fits-all condition, and this is especially true after age 65. By 2026, approximately 74% of adults over 65 in the United States are estimated to have hypertension, according to updated CDC surveillance data. In South Korea, the National Health Insurance Service (NHIS) reports that nearly 6 in 10 adults over 60 are actively managed for hypertension-related conditions.
But here’s the nuance most general health articles skip over: older adults experience something called isolated systolic hypertension (ISH) — where the top number (systolic) is high, but the bottom (diastolic) may actually be normal or even low. This pattern is driven by arterial stiffness, a natural consequence of aging. Treating it aggressively like you would in a 45-year-old can actually increase the risk of falls, kidney injury, and even cognitive decline.
What the 2026 Guidelines Actually Say
The American College of Cardiology (ACC) and the American Heart Association (AHA) updated their joint hypertension guidelines in late 2025, with full implementation recommendations rolling out into clinical practice in early 2026. Here are the key takeaways that matter most for older adult care:
- Target blood pressure for adults 65–79: The updated consensus now recommends a systolic target of <130 mmHg for most patients in this group — but with important caveats around frailty and polypharmacy (taking multiple medications simultaneously).
- Adults 80 and older: The target has been relaxed slightly to <140 mmHg systolic, acknowledging that overly aggressive treatment in this population correlates with higher rates of orthostatic hypotension (a sudden drop in blood pressure when standing up).
- Individualized assessment is now mandatory: The 2026 framework explicitly requires a frailty score and a cognitive assessment as part of hypertension management planning for patients over 70. This is a big shift from the one-number-fits-all approach.
- Home blood pressure monitoring (HBPM): Validated as the gold standard over white-coat readings. Patients are now encouraged to take readings twice daily for 7 consecutive days before any medication change.
- Lifestyle intervention timelines: A 3-month structured lifestyle modification window is now formally recommended before initiating pharmacotherapy in Stage 1 hypertension (130–139/80–89 mmHg) for lower-risk older adults.
The SPRINT SENIOR Data Revisited — What It Means in Practice
You’ve probably heard of the SPRINT trial — the landmark study that reshaped blood pressure targets. What’s interesting in 2026 is how researchers have continued to mine the older adult subgroup data (SPRINT SENIOR). The key finding that’s now influencing clinical decisions: intensive treatment (<120 mmHg systolic) reduced cardiovascular events by roughly 34% in ambulatory, non-frail seniors, but the benefit largely disappeared — and harm risk increased — in frail individuals with slow gait speed or low grip strength.
This is why your doctor might now be asking you to walk across the room or squeeze a grip dynamometer during a routine blood pressure visit. It’s not random — it’s part of the Comprehensive Geriatric Assessment (CGA) framework that’s being integrated into hypertension care in 2026.
Real-World Examples: What Different Countries Are Doing
It’s genuinely fascinating to look at how different healthcare systems are operationalizing these guidelines. Let’s explore a few:
South Korea (한국): The Korean Society of Hypertension updated its clinical guidelines in January 2026 to align closely with the ACC/AHA framework, but added culturally specific recommendations around sodium intake — a pressing issue given that traditional Korean diets can involve significantly high sodium through fermented foods like kimchi and doenjang. Community health centers (보건소) are now running tailored low-sodium cooking workshops specifically for adults over 65, with measurable reduction in average systolic readings of 4–6 mmHg in pilot cohorts in Seoul and Busan.
Japan: The Japanese Society of Hypertension has taken a particularly nuanced stance on the 80+ age group, favoring a systolic target of <150 mmHg for “robust elderly” and <160 mmHg for frail patients — slightly more conservative than Western targets. Japan’s integrated community care system (地域包括ケアシステム) embeds pharmacists and nurses directly in senior living communities to monitor BP and flag concerns before hospitalization is needed.
United Kingdom: NHS England’s 2026 hypertension pathway for older adults now includes a mandatory annual “medication review” for all patients over 75 on antihypertensives, with a focus on deprescribing (strategically reducing unnecessary medications) when blood pressure is well-controlled and fall risk is elevated. This has reduced adverse drug events in this population by an estimated 12% according to NHS Digital’s early 2026 report.
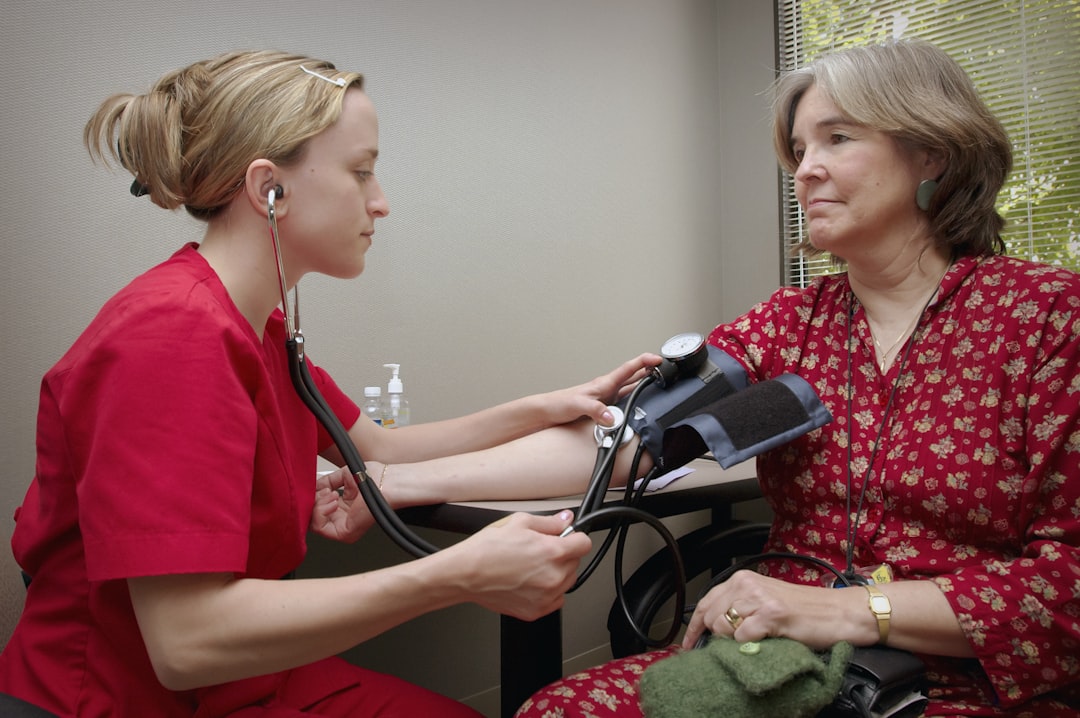
The Lifestyle Piece — Still Underrated, Still Powerful
Before we go deep into medication strategies, let’s be honest about something: lifestyle modification remains extraordinarily effective, even in older adults — and it’s often underutilized. Here’s a quick breakdown of what the evidence supports in 2026:
- DASH Diet adherence: Can lower systolic BP by 8–14 mmHg. Even partial adherence (2–3 changes rather than full overhaul) shows meaningful benefits in seniors.
- Sodium reduction: Reducing intake from 3,500 mg/day to under 2,300 mg/day typically reduces systolic BP by 4–8 mmHg in salt-sensitive individuals (older adults tend to be more salt-sensitive).
- Resistance training: Often overlooked in favor of aerobic exercise — but 2025–2026 meta-analyses confirm that moderate resistance training 2–3x/week reduces systolic BP by approximately 4 mmHg and improves vascular compliance in adults over 65.
- Stress reduction and sleep quality: Chronic poor sleep now has its own dedicated section in the 2026 hypertension guidelines as a modifiable risk factor. Adults sleeping fewer than 6 hours consistently show 20–30% higher cardiovascular event rates.
- Alcohol moderation: Even moderate drinking (>7 drinks/week) is now more firmly linked to resistant hypertension in older adults — this is an area where guidance has tightened considerably.
Medications in 2026: What’s Changed?
The core medication classes haven’t changed dramatically, but how they’re being used — and for whom — is being refined. The preferred first-line agents for older adults remain:
- Thiazide-type diuretics (like chlorthalidone, which is now preferred over hydrochlorothiazide based on accumulated evidence)
- CCBs (Calcium Channel Blockers) — particularly amlodipine — remain excellent for isolated systolic hypertension
- ACE inhibitors or ARBs — especially when diabetes or kidney disease is co-present
What’s new? There’s growing real-world use of single-pill combination therapy (SPC) in older adults — combining two or three drugs in one tablet. The compliance data is compelling: SPCs improve adherence by 20–30% compared to taking multiple separate pills, which matters enormously when you’re managing multiple conditions at once (a reality for most seniors).
Also worth watching: renal denervation — a minimally invasive procedure where specific nerves around the kidneys are disrupted to reduce BP signals — has received expanded approval in several markets by early 2026 for truly resistant hypertension cases where medications aren’t working. It’s not mainstream yet for seniors, but it’s on the horizon.
Practical Tips for Older Adults and Their Caregivers Right Now
- Invest in a validated home blood pressure monitor (look for the dabl Educational Trust or BHS validation certification). Measure twice daily at the same time — morning before medication, evening before bed.
- Keep a BP log (an app or even a paper chart works) and bring it to every appointment. This data is gold for your doctor.
- Ask your doctor specifically: “Is my BP target appropriate for my age and frailty level?” This opens the door to a more individualized conversation.
- If you’re experiencing dizziness when standing, report it immediately — this could be orthostatic hypotension, which is treatable and a fall risk.
- Review all medications (including over-the-counter NSAIDs like ibuprofen) with your pharmacist — several common drugs can raise blood pressure or interfere with antihypertensives.
Realistic Alternatives When the Standard Path Isn’t Working
Not every older adult can follow a strict DASH diet, afford new medications, or tolerate aggressive BP lowering. Here’s where thinking through realistic alternatives becomes important:
If medication side effects are a barrier, ask about dose titration — starting at half the standard dose and gradually increasing is now explicitly supported in the 2026 guidelines for adults over 75. If dietary changes feel overwhelming, a single targeted change (like cutting processed foods and restaurant meals, which account for ~70% of sodium intake for most Americans) can deliver meaningful results without a complete lifestyle overhaul.
For caregivers of seniors with cognitive decline, remote patient monitoring tools — including Bluetooth-enabled BP cuffs that automatically sync to a healthcare portal — have become far more accessible and affordable in 2026, making it easier to keep clinicians informed without burdening the patient with complex technology.
And perhaps most importantly: if you’re feeling like your current treatment plan is just being repeated on autopilot at each annual visit, it’s completely reasonable to ask for a referral to a geriatric cardiologist or a clinical pharmacist specializing in older adult care. The field has moved — your care plan should too.
Editor’s Comment : What strikes me most about where we are in 2026 is that hypertension care for older adults is finally becoming genuinely personalized — not just in theory, but in actual clinical practice. The days of chasing a single magic number regardless of context are fading. The real win here is recognizing that for Margaret, and for millions like her, the goal isn’t just a lower reading on a monitor — it’s more mornings without dizziness, more years of independence, and more quality time with the people she loves. That’s the number we should all be optimizing for.
태그: [‘elderly hypertension management 2026’, ‘high blood pressure older adults’, ‘senior cardiovascular health’, ‘hypertension guidelines 2026’, ‘blood pressure treatment aging’, ‘geriatric hypertension care’, ‘DASH diet seniors blood pressure’]